Many autistic people rely on important healthcare coverage from Medicaid for continued services and supports throughout their life. But when entering adulthood, autistic adolescents are facing increased risk of disenrollment from the Medicaid program if they live in a state without a Medicaid waiver. Recently published in JAMA Network Open, researchers from the A.J. Drexel Autism Institute at Drexel University examined whether state-level waivers were associated with reduced risk of Medicaid disenrollment among autistic transition-age youth.
Being insured is important because it is associated with fewer unmet healthcare needs and lower healthcare expenses for families. Medicaid waivers have targeted eligibility criteria based on age and/or diagnosis for specific populations that allow states to provide needed services, including to autistic people. Most states provide services to autistic youth through 1915(c) waivers, which provide healthcare services in home- and community-based settings rather than more restrictive settings.
“We found that autistic adolescents living in a state with any kind of 1915(c) Medicaid waiver had a better chance of remaining enrolled in Medicaid as they entered adulthood,” said Meghan Carey, a doctoral student in the Epidemiology department in the Dornsife School of Public Health, and lead author.
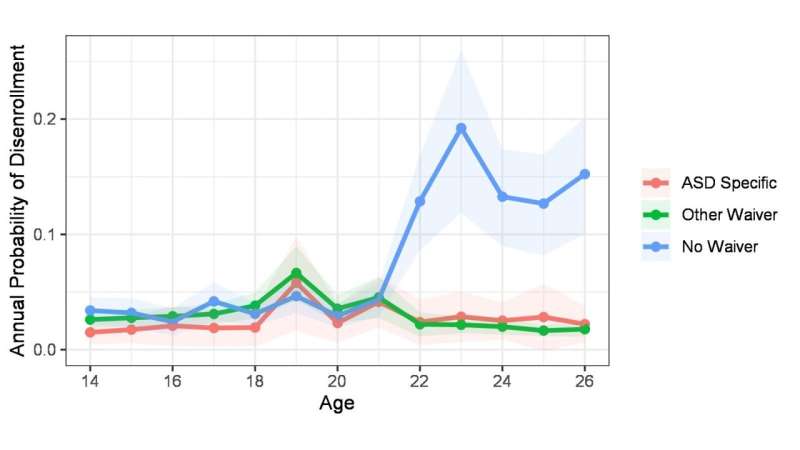
Researchers found that from age 14 through 21, there was little difference in the probability of disenrollment across states. But at age 22, the probability of disenrollment in states without waivers increased dramatically to more than 13%—whereas it remained stable (about 2%) for those in states with a waiver.
“We also found that compared to autistic young people who are continuously enrolled in Medicaid, a higher proportion of autistic young people who experience disenrollment were Medicaid-eligible due to poverty,” said Carey.
Carey added that findings supported the notion that requirements for remaining continuously enrolled in Medicaid when poverty-eligible may be challenging because small changes in income can result in disenrollment.
The study included 14,739 autistic individuals who experienced disenrollment from Medicaid and 119,216 continuously enrolled autistic individuals. The research team extracted data from Medicaid records from 2008–2016, from 47 states and Washington, DC. Arizona, Rhode Island and Vermont use a different waiver mechanism (Section 1115 waivers which are more broad in scope and reach more constituents compared to 1915(c) waivers) and were excluded.
“Interestingly, autism-specific waivers were not associated with greater decreases in disenrollment for autistic transition-age youth compared with waivers with other diagnosis or functional eligibility criteria,” said Carey. “This suggests that for purposes of mitigating disenrollment among autistic transition-age youth, autism-specific waivers may not be necessary.”
Carey and her research team noted that policymakers should consider bolstering continuity of waiver availability to keep autistic transition-age youth insured and connected to necessary healthcare services, which could improve health-related and other outcomes for autistic adults, or explore other eligibility mechanisms for Medicaid.
More information:
Meghan E. Carey et al, Association Between Medicaid Waivers and Medicaid Disenrollment Among Autistic Adolescents During the Transition to Adulthood, JAMA Network Open (2023). DOI: 10.1001/jamanetworkopen.2023.2768
Journal information:
JAMA Network Open
Source: Read Full Article


