A genetic study has identified neuronal abnormalities in the electrical activity of cortical cells derived from people with a rare genetic disorder called 22q11.2 deletion syndrome. The overexpression of a specific gene and exposure to several antipsychotic drugs helped restore normal cellular functioning. The study, funded by the National Institutes of Health (NIH) and published in Nature Medicine, sheds light on factors that may contribute to the development of mental illnesses in 22q11.2 deletion syndrome and may help identify possible targets for treatment development.
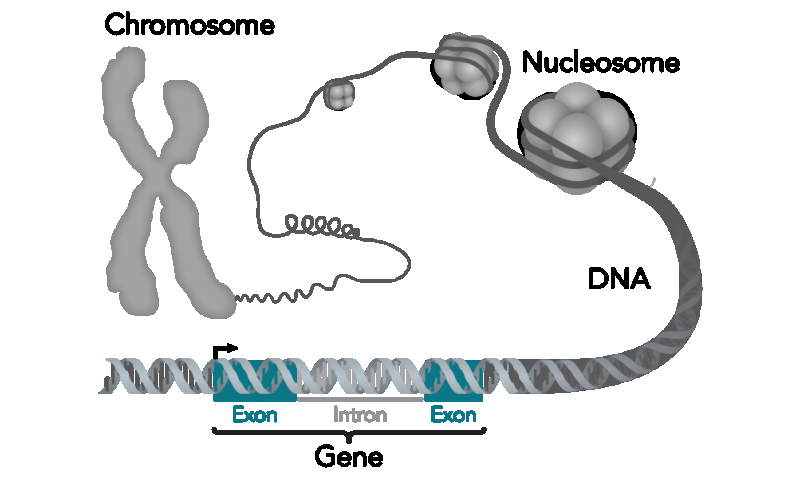
22q11.2 deletion syndrome is a genetic disorder caused by the deletion of a piece of genetic material at location q11.2 on chromosome 22. People with 22q11.2 deletion syndrome can experience heart abnormalities, poor immune functioning, abnormal palate development, skeletal differences, and developmental delays. In addition, this deletion confers a 20-30% risk for autism spectrum disorder (ASD) and an up to 30-fold increase in risk for psychosis. 22q11.2 deletion syndrome is the most common genetic copy number variant found in those with ASD, and up to a quarter of people with this genetic syndrome develop a schizophrenia spectrum disorder.
“This is the largest study of its type in terms of the number of patients who donated cells, and it is significant for its focus on a key genetic risk factor for mental illnesses,” said David Panchision, Ph.D., chief of the Developmental Neurobiology Program at the NIH’s National Institute of Mental Health. “Importantly, this study shows consistent, specific patient-control differences in neuronal function and a potential mechanistic target for developing new therapies for treating this disorder.”
While some effects of this genetic syndrome, such as cardiovascular and immune concerns, can be successfully managed, the associated psychiatric effects have been more challenging to address. This is partly because the underlying cellular deficits in the central nervous system that contribute to mental illnesses in this syndrome are not well understood. While recent studies of 22q11.2 deletion syndrome in rodent models have provided some important insights into possible brain circuit-level abnormalities associated with the syndrome, more needs to be understood about the neuronal pathways in humans.
To investigate the neural pathways associated with mental illnesses in those with 22q11.2 deletion syndrome, Sergiu Pasca, M.D., associate professor of psychiatry and behavioral sciences at Stanford University, Stanford, California, along with a team of researchers from several other universities and institutes, created induced pluripotent stems cells—cells derived from adult skin cells reprogramed into an immature stem-cell-like state—from 15 people with 22q11.2 deletion and 15 people without the syndrome. The researchers used these cells to create, in a dish, three-dimensional brain organoids that recapitulate key features of the developing human cerebral cortex.
“What is exciting is that these 3-D cellular models of the brain self-organize and, if guided to resemble the cerebral cortex, for instance, contain functional glutamatergic neurons of deep and superficial layers and non-reactive astrocytes and can be maintained for years in culture. So, there is a lot of excitement about the potential of these patient-derived models to study neuropsychiatric disease,” said Dr. Pasca.
The researchers analyzed gene expression in the organoids across 100 days of development. They found changes in the expression of genes linked to neuronal excitability in the organoids that were created using cells from individuals with 22q11.2 deletion syndrome. These changes prompted the researchers to take a closer look at the properties associated with electrical signaling and communication in these neurons. One way neurons communicate is electrically, through controlled changes in the positive or negative charge of the cell membrane. This electrical charge is created when ions, such as calcium, move into or out of the cell through small channels in the cell’s membrane. The researchers imaged thousands of cells and recorded the electrical activity of hundreds of neurons derived from individuals with 22q11.2 deletion syndrome and found abnormalities in the way calcium was moved into and out of the cells that were related to a defect in the resting electrical potential of the cell membrane.
A gene called DGCR8 is part of the genetic material deleted in 22q11.2 deletion syndrome, and it has been previously associated with neuronal abnormalities in rodent models of this syndrome. The researchers found that heterozygous loss of this gene was sufficient to induce the changes in excitability they had observed in 22q11.2-derived neurons and that overexpression of DGCR8 led to partial restoration of normal cellular functioning. In addition, treating 22q11.2 deletion syndrome neurons with one of three antipsychotic drugs (raclopride, sulpiride, or olanzapine) restored the observed deficits in resting membrane potential of the neurons within minutes.
Source: Read Full Article


