
Already available in over 100 countries, Nexplanon is now finally approved for use in Canada. Nexplanon is a contraceptive implant: a small rod, inserted into the upper arm through a tiny incision, that prevents pregnancy for up to three years.
It works by releasing a very low continuous dose of a synthetic progesterone. The contraceptive implant offers an important and overdue addition to contraception options for patients in Canada.
Nexplanon’s long-awaited arrival could not be more opportune, as COVID-19 has demonstrated just how much patients need flexibility and choices to meet the essential need for access to contraception.
Long-acting reversible contraception
Up until now, hormonal or copper intrauterine devices (IUDs) were the only truly long-acting reversible contraception (LARC) available in Canada.
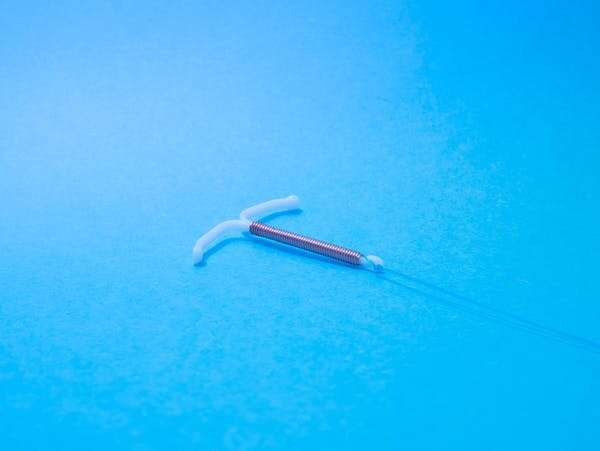
An IUD is a small T-shaped object inserted through the cervix into the uterus. Hormonal IUDs also work by slowly releasing synthetic progesterone. Both the IUD and Nexplanon are highly effective at pregnancy prevention when in place, and the potential to become pregnant resumes immediately when they are removed.
Patients may prefer LARC over other types of contraceptives because life, school, work and other factors make daily or weekly options untenable at the best of times. Irregular work schedules can be incompatible with taking a pill every day at the same time. Seasonal employment and jobs away from home can limit physical and financial ability to seek prescription renewals. And contraceptives taken frequently are more difficult to hide from controlling sexual partners or disapproving parents.

LARC benefits
For some patients it is simply too hard to remember daily pills or weekly patches—the pandemic has demonstrated just how difficult some circumstances can make it to maintain a regular schedule. LARC offers three or more years of uninterrupted, effective pregnancy prevention.
The contraceptive implant also offers an alternative to a device that is inserted vaginally. Some patients have concerns or anxiety about the potential for pain during the IUD insertion process.
Pelvic exams may be triggering for survivors of sexual assault. Some patients may be uncomfortable with the idea of having the IUD remain in place in their uterus. For these patients, Nexplanon provides an alternative.
Timely and effective
Nexplanon also provides an effective and timely long-term contraceptive option following an abortion. One of the optimal times to place an IUD is at the end of a surgical abortion procedure, when the cervix is dilated, medications have been provided to reduce anxiety and pain, and an IUD is easily inserted. However, this only works for patients seeking surgical abortion.
In 2017, Mifegymiso, the abortion pill, became widely available in Canada as a method to induce abortion at home. Since then, an increasing proportion of patients are choosing medical abortion (an abortion using medication) over surgical abortion.
Patients who choose medical abortion and want an IUD need to return to clinic for the insertion after their abortion at home is complete. This results in a delay and the need to book a subsequent appointment. The wait increases their risk of unplanned pregnancy.
These patients may not ever get their chosen contraception, as many barriers impede following through with that followup visit. This is especially true in Canada, where rural and urban access to abortion and reproductive health services remains decidedly unequal. During COVID-19, reproductive health patients have faced reduced service availability, limited clinic hours, and a shift towards provision of care by phone. Nexplanon, however, could be inserted in the arm when the patient comes in for a prescription for medical abortion pills.
Contraception costs
We do not yet know how the cost of Nexplanon will compare to the IUD or other contraceptive options. Ideally, Nexplanon—and all contraception—should be covered by provincial health insurance. Such coverage would prevent the high costs—individual and system, direct and indirect—of accidental pregnancies.

One of the greatest barriers to effective contraception use is cost to the patient. Yet both surgical and medical abortion is almost universally covered in every province and territory in Canada. The arrival of the contraceptive implant is an opportunity for provinces and territories to step up and assume responsibility for making reproductive health options like LARCs financially accessible to all.
Nexplanon, like IUDs, will not prevent sexually transmitted infections (STIs). Barrier methods such as condoms remain necessary to prevent infection. Perhaps our enthusiastic embrace of infection prevention information and practices during COVID-19 will extend to understanding STIs, destigmatizing testing and encouraging effective prevention.
Source: Read Full Article


